State watchdog: New Jersey nursing home owners skimmed millions while residents suffered
New: N.J. nursing home owners diverted millions while residents suffered, state says
A sweeping state investigation by the Office of the State Comptroller has found two South Jersey nursing homes siphoned tens of millions in Medicaid dollars into a maze of family-controlled companies while residents endured unsafe understaffing, neglect, and life-threatening lapses in care.
The big picture
New Jersey’s top watchdog says Hammonton Center and Deptford Center are not outliers but symptoms of a systemic crisis in long-term care. The homes operated with half the staff required by law while their owners concealed financial transactions with companies they and their relatives controlled.
Why it matters
Residents weren’t simply underserved. They were put in danger.
- Police received 3,400+ calls from the two homes.
- Residents went without medications, hygiene, and basic supervision.
- One resident died after staff disregarded his dietary care plan.
- Many endured hours-long waits as call bells rang unanswered.
State officials say the pattern reflects a business model that rewards profit extraction, not care.
Kevin Walsh, Acting State Comptroller:
“Rampant profiteering leads to poor quality care and often misery as the most vulnerable people in our society press call buttons and scream for help without anyone answering, hour after hour, day after day, year after year, not because New Jersey and the federal government have not paid for their care. Society has done its part through the Medicaid program.”
” The call bells and the screams go unanswered because Kenneth Rosenberg, Darryl Hagler, and the other owners of nursing homes have built sophisticated systems that extract wealth from taxpayers through related party schemes that enrich themselves while hollowing out care. And New Jersey government has thus far been ineffective at mounting a comprehensive, effective response that protects residents and the Medicaid funds from nursing home owners who are willing to break the rules to make more money.”
Driving the news
The Office of the State Comptroller found that owners Daryl Hagler and Kenneth Rozenberg:
- diverted $92 million to companies run by themselves, their children, in-laws, and associates
- reported less than 1% of those transactions to regulators
- used inflated mortgages to justify excessive rent
- left residents with staffing levels far below legal minimums
Walsh: “They got rich off the backs of people who were unable to care for themselves.”
📊 By the numbers
- Almost 52% — Hammonton’s average understaffing
- Average of 54% — Deptford’s average understaffing
- 2,400+ — police calls from Deptford
- 1,000+ — police calls from Hammonton
- $42.1M — Medicaid overpayment tied to illegal staffing at Hammonton
- $44.2M — same at Deptford
- $980,000 — penalties for failing to staff the required registered nurses
- $123.9M — total recovery the state is seeking
How the scheme worked
According to the comptroller:
1. Create dozens of related companies
Staffing firms, labs, IT providers, management companies — all owned by family members or close associates.
2. Route nursing-home payments into them
The homes paid inflated or improper fees to these insider entities.
3. Hide the transactions
Only $882,666 of $92 million in related-party payments appeared on mandatory cost reports.
4. Inflate rent through oversized mortgages
Hagler and Rozenberg borrowed far beyond property value, then charged rent tied to the inflated debt.
5. Move profits into private accounts
Tens of millions flowed into LLCs controlled by the owners and their families.
Walsh: “They created illegitimate profit centers disguised as rent.”
What they’re saying
Walsh:
“Instead of providing even the bare minimum care, they maximized their profits at the expense of residents.”
Laurie Brewer, Long-Term Care Ombudsman:
“This is an absolute bombshell. The financial trickery and substandard care sickens me.”
Brewer on reform:
“When a nursing home is routinely understaffed, we shouldn’t just fine them. We should shut down their admissions.”
Walsh on legislative inaction:
“Report after report, both in New Jersey and nationally, has shown the extent of the problem. We issued a report one year ago that showed an astounding siphoning of public funds occurring in South Jersey Extended Care in Bridgeton, a nursing home owned by a straw owner that was in a network of 10 nursing homes. We made recommendations to the legislature and state agencies…The legislature did pretty much nothing. There was a single hearing on a bill in the Senate, but no laws were passed, and when the Department of Human Services earlier this year instituted a program that would cut off funding for new admissions and bad nursing homes that fail to improve, the program, without any debate, was abolished in the budget in June 2025. That was a sad moment for New Jersey, and for the residents of New Jersey nursing homes.”
AARP-NJ State Director Chris Widelo:
“This is not mismanagement – it is a systemic, dangerous breakdown in oversight and accountability that is putting residents’ lives at risk while operators enrich themselves at taxpayer expense.”
The reform that has stalled: S-1948
A bill sponsored by Sen. Joe Vitale would:
- require audited financial statements
- mandate full ownership and related-party disclosure
- expand oversight to entire chains
- strengthen scrutiny of operators with poor records
Instead of regulating nursing home operators, the state keeps rewarding them with rate increases, with no transparency. In the fiscal year 2025-26 budget, the Legislature overrode regulations published last year that permitted those who manage Medicaid to stop payments to nursing homes that have been cited for major deficiencies by inspectors or that receive one-star ratings in nine of the last 12 quarters.
Brewer: “The Legislature keeps shoveling money at these nursing homes but won’t pass this transparency bill.”
Walsh: “The facts we uncover in this report cry out for state government, including the Legislature, to finally recognize that New Jersey nursing homes are straining under the weight of fraud, waste, and abuse. The problem isn’t limited to just a few nursing homes. This problem is systemic, uncontrolled, and shows no signs of getting better.”
AARP-NJ State Director Chris Widelo:
“The Legislature must act. AARP New Jersey is calling for the immediate passage of S1948/A1872, which would require full financial transparency, including disclosure of all owners and related-party companies, through audited, consolidated financial statements. Without the ability to follow the money, New Jersey cannot protect residents or hold operators accountable…Today’s report makes one thing painfully clear: nursing home residents are living in unsafe conditions, operators are exploiting financial loopholes for profit, and taxpayers are footing the bill. This must end. Lawmakers must pass S1948/A1872 now.”

Two South Jersey nursing homes operated by a pair of long-term care investors diverted tens of millions of Medicaid dollars away from resident care and into a sprawling web of companies they and their relatives controlled, according to an investigation detailed in a new report by the New Jersey Office of the State Comptroller.
The findings, released after an investigation of activity at the nursing homes from 2019 to 2024, detail chronic understaffing, falsified financial disclosures, inflated rents and mortgage structures, and widespread neglect at Hammonton Center for Rehabilitation and Healthcare in Atlantic County and Deptford Center for Rehabilitation and Healthcare in Gloucester County. Both facilities housed hundreds of residents, most of them Medicaid beneficiaries, while owners extracted money intended to support adequate staffing, medical care, and safe living conditions.
“All indications are that what we have identified in this and in earlier reports is just the tip of the iceberg in the nursing home industry,” State Comptroller Kevin Walsh said. “The findings in this report, unfortunately, are not unique. Ingrained self-dealing, routine siphoning, profit taking to the detriment of residents, and the overall lack of transparency and accountability present here is the business model used by many New Jersey nursing homes.”
State investigators concluded that nursing home owners Daryl Hagler and Kenneth Rozenberg, longtime business partners who control 46 nursing homes across four states, “grievously harmed” residents and misled state and federal regulators by concealing the scale of their self-dealing. The report describes how the pair used a constellation of related companies run by themselves, their children, their in-laws, and associates to extract $92 million from the two New Jersey nursing homes.
“When presented with those findings, they told us pretty much, well, it’s fine, because everyone does it,” Walsh said.
The comptroller is seeking to recover at least $123.9 million in overpayments, penalties, and improperly spent Medicaid funds from the owners and their related entities.
“They concealed these transactions in the hope that no one would notice just how much they were exploiting the residents and profiteering at the expense of taxpayers,” Walsh said. “They got rich off the backs of people who were unable to care for themselves, who were sick, elderly, and disabled.”
Chronic understaffing
Chronic, sustained understaffing at the two facilities “provided something entirely different” from what taxpayers paid for, according to the Office of the State Comptroller.
Investigators reviewed 146 randomly selected days between 2021 and 2024 and found that both Hammonton and Deptford violated New Jersey’s minimum staffing law nearly every day. On average:
- Hammonton was understaffed by almost 52 percent.
- Deptford was understaffed by 54 percent, on average.
“Residents in both facilities received less than half the minimum of direct care they were required by law to receive,” Walsh said.
Both facilities routinely operated without a registered nurse on duty, even though state law requires 24-hour RN coverage in large nursing homes. Instead, licensed practical nurses who cannot legally perform RN-level duties were placed in charge, sometimes overnight and without supervision.
The resulting care failures included missed medications, unmonitored blood sugar, untreated wounds, and hours-long delays for basic hygiene assistance. In one case, a resident with acute medical needs went without 15 essential medications for more than a week. In another case, a resident who required a pureed diet died after staff fed him solid food in violation of his care plan.
In 2023, state inspectors found a resident wearing an identification badge soaked in urine and mildew. That same year, the Department of Health temporarily froze admissions at Hammonton, citing “immediate and serious threats of harm” tied to inadequate nurse staffing.
Walsh said these failures were driven not by statewide workforce shortages but by ownership’s financial strategy. “Instead of providing even the bare minimum care, they maximized their profits at the expense of the residents,” he said.
Crying for help

Police responded to more than 2,400 calls from Deptford and about 1,000 from Hammonton during the review period. Many came from residents who said they had no one else to turn to. Officers described entering buildings where call bells blared unanswered, and residents pleaded for assistance.
In one case, a Hammonton resident repeatedly called 911 because his tongue was swelling dangerously, and staff refused to send him to a hospital. A responding officer, after seeing the condition firsthand, called an ambulance on the resident’s behalf.
A volunteer who visited Deptford Center weekly over several years told state investigators the nursing home was chronically unsanitary and unsafe, with residents routinely left without basic care. The volunteer described the building as “disgusting,” citing dirty floors and bathrooms, foul odors, extreme temperatures, and poor hygiene conditions. The volunteer said that staff members often failed to meet residents’ basic needs, leaving them thirsty, hungry, unattended, and in soiled clothing for long periods.
The volunteer reported witnessing repeated neglect and provided photographs to corroborate the observations. Among them:
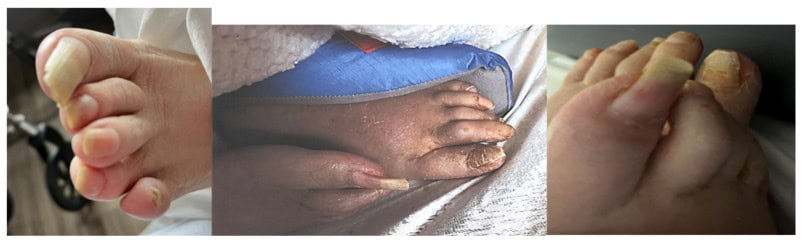
- Severe grooming neglect: Two residents’ toenails had grown so long they curled over their toes. When the volunteer raised concerns, staff said a podiatrist visits only once a month.
- Disabled call bell: On Nov. 21, 2023, the volunteer found a resident’s call bell cord severed, leaving the resident unable to summon help.
- Rooms contaminated with waste: The volunteer described one resident’s room as smelling strongly of urine and feces. Photos showed a fallen meal tray mixed with dirty diapers, used diapers discarded on the floor, and food left scattered on the ground for long stretches of time.
- Food safety hazards: On Feb. 1, 2024, the volunteer photographed flies on a resident’s meal tray.
- Untreated incontinence: On Sept. 19, 2023, the volunteer found a resident sitting in her own excrement in the middle of the day, with dried feces in her hand. Staff claimed the resident had just been cleaned, a statement the volunteer believed was inconsistent with what they saw.
The volunteer’s reports echoed accounts from families quoted in a May 2024 news investigation into conditions at Hammonton Center, where one daughter described dehydration, missed or incorrect medical care, and long stretches without staff present. “Understaffed is an understatement,” she said. “You could see her decline every time we visited her.”
A family quoted in a May 2024 news article said they watched their mother deteriorate during her stay at Hammonton. “Understaffed is an understatement,” the daughter told reporters. “You could see her decline every time we visited her.”
How the scheme worked
- Inflate costs through related-party companies
The owners created dozens of related companies — including staffing agencies, management firms, laboratories, IT providers and property companies — controlled by themselves, their children, in-laws and close associates. - Charge the nursing homes inflated or improper fees
Instead of using independent vendors, the facilities paid these insider companies inflated or nonallowable fees, violating Medicaid rules that require related-party costs to reflect actual expenses. - Hide the transactions
The owners reported less than 1 percent of related-party spending on required cost reports, concealing the flow of money to entities they controlled. - Use inflated mortgages to justify excessive rent
The owners borrowed far beyond the property values and then charged the nursing homes rent based on the inflated debt. They refinanced through federal housing loans, preserving the rent structure and masking business acquisition costs as property expenses. - Move profits into private accounts
Tens of millions of dollars flowed through limited liability companies controlled by the owners and their families, generating substantial profits while reducing funds available for resident care.
The Office of the State Comptroller concluded the structure was designed to extract public money while disguising private enrichment as legitimate operating expenses.
Related-party empire, hidden profits
Between 2019 and 2024, the two nursing homes paid $92 million to a constellation of related companies. These included:
- Centers for Care LLC, the owners’ Bronx-based management company, which received more than $27 million.
- Property companies owned by Rozenberg and KFE that collected inflated rent.
- Staffing agencies owned by the owners’ daughters and sons-in-law.
- Business, IT, and maintenance companies registered to family members.
- Clinical labs owned by Rozenberg and his wife.
Hagler and Rozenberg disclosed just $882,666 of these payments on mandatory cost reports.
“They effectively used Medicaid money to fund the purchase of their business,” Walsh said. “This saddled the nursing home and the Medicaid program with years and years of excessive rent payments for a mortgage that was double what it should have been.”
Their accounting firm falsely told regulators that Centers for Care had no related-party entities beyond two minor companies, according to the Office of the State Comptroller.
Investigative reporting by New Jerseyans for New Jerseyans. Help us uncover untold stories in New Jersey. Donate to our nonprofit newsroom today.
HUD-backed refinancing and inflated rents
In 2014, the owners purchased Hammonton, Deptford, and a third New Jersey nursing home using a $58.2 million mortgage, even though the properties themselves cost just $20.6 million. The inflated mortgage financed the purchase of the operating businesses, allowing the owners to charge higher rent based on debt unrelated to the buildings.
In 2017, they refinanced again, securing $63.2 million in U.S. Department of Housing and Urban Development–backed loans. The refinancing provided federal protection while preserving inflated rental obligations.
Under these arrangements:
- Base rent doubled from about $1.1 million to more than $2.2 million annually.
- “Additional rent” ballooned to more than $31.6 million.
- About $27.8 million went directly to Rozenberg’s property companies.
- At least $7.8 million covered non-property business costs improperly.
Walsh described the structure bluntly: “They created illegitimate profit centers disguised as rent, shifting private business costs onto Medicaid.”
Overpayments tied to days of no legal staffing
The Office of the State Comptroller calculated that:
- Hammonton was overpaid $42.1 million.
- Deptford was overpaid $44.2 million.
- Registered nurse staffing penalties totaled $980,000.
“Can you imagine if the tens of millions of dollars siphoned away as so-called rent went to improve the quality of care by having more staffing?” Walsh said. “If that money went into caring for residents and respecting employees, we’d be in a very different spot.”
Oversight failures
The report is not just an indictment of Hagler and Rozenberg. It also highlights systemic problems in New Jersey’s long-term care oversight system.

Long-Term Care Ombudsman Laurie Brewer, whose office has long raised concerns about both facilities, called the comptroller’s findings “a bombshell.”
“The financial trickery and substandard care at these nursing homes sickens me,” Brewer said. “The public deserves to know where every dollar went, and the harsh truth is that we really don’t. Many nursing homes routinely divert money away from resident care and into the pockets of owners and owners’ families.”
Brewer said the state must take stronger action.
“When a nursing home is routinely understaffed, we shouldn’t just fine them. We should shut down their admissions. We shouldn’t allow them to take in new residents when they can’t care for the ones they have,” she said.
She also called for more staff and resources inside the Department of Health, the Department of Human Services, and the Medicaid Fraud Division.
“This is incredibly labor-intensive work,” she said. “It’s painstaking, difficult work. And nobody wants to do it.”
Walsh said his office has repeatedly detailed how nursing home operators divert public funds while residents suffer. “The Legislature did pretty much nothing,” he said.
What New Jersey Senate Bill S-1948 would do
Sponsored by Sen. Joe Vitale, S-1948 would strengthen financial transparency in nursing homes by:
- Requiring audited financial statements for every nursing home and all related entities.
- Mandating full disclosure of ownership and related-party structures.
- Increasing the state’s ability to review entire nursing home chains, not just individual facilities.
- Improving oversight so that operators with poor track records cannot expand without scrutiny.
Brewer and Walsh both said the reforms are essential in order to expose the kind of hidden financial practices uncovered at Hammonton and Deptford.
The Office of the State Comptroller said that greater transparency, including audited financial statements and full disclosure of related-party transactions, would have allowed regulators to detect the misconduct far earlier.
A powerful industry, persistent legislative inaction

New Jersey’s for-profit nursing home industry has long been a powerful presence in state politics. While the Office of the State Comptroller report does not address lobbying or campaign spending, advocates and watchdogs have repeatedly pointed to the industry’s influence as one reason transparency reforms have stalled in Trenton.
In recent years, lawmakers have failed to advance measures that would strengthen financial oversight, tighten controls on related-party transactions and improve enforcement of minimum staffing laws.
Walsh noted that his office has issued multiple reports documenting widespread financial abuses in nursing homes with little response from the Legislature. “The Legislature did pretty much nothing,” he said.
Brewer said the dynamic has left residents unprotected and that real reform is needed. The misconduct detailed in the report, she said, translates directly into human harm.
“The Legislature keeps shoveling money at these nursing homes, but won’t pass this transparency bill. I call for them to do that right away,” she said.
“When we talk about millions of dollars being siphoned into the owner’s pockets, there is real human misery at the end of that equation. The long-term system we have created to care for people with disabilities, people who are sick, people who are elderly in these long-term care facilities, is broken.”
AARP New Jersey, a longtime advocate for reform at the state’s more than 340 nursing homes, responded swiftly to the findings of the Office of the State Comptroller report.
State Director Chris Widelo said the report exposes a level of dysfunction and lawlessness in New Jersey’s nursing homes that is “nothing short of shocking.”
“This is not mismanagement – it is a systemic, dangerous breakdown in oversight and accountability that is putting residents’ lives at risk while operators enrich themselves at taxpayer expense,” Widelo said.
“The report details horrific incidents – including the death of a resident, two sexual assaults, and thousands of 911 calls from inside facilities that are supposed to be providing care. These are the most vulnerable people in our state, and they are being failed at every turn,” Widelo said.
New Jersey spends more than $2 billion a year on nursing homes, yet many facilities continue to be understaffed, underperform, and endanger residents, Widelo said. He noted that since the 2022 fiscal year, nursing homes have received more than $250 million in additional state funding with no added transparency requirements.
“Taxpayers are being forced to subsidize poor care, dangerous conditions, and hidden profits,” Widelo said.
AARP New Jersey is calling for the immediate passage of Senate Bill S-1948, sponsored by Sen. Joe Vitale.
“Without the ability to follow the money, New Jersey cannot protect residents or hold operators accountable,” Widelo said. “Today’s report makes one thing painfully clear: nursing home residents are living in unsafe conditions, operators are exploiting financial loopholes for profit, and taxpayers are footing the bill. This must end.”
If this reporting helped you understand something important about New Jersey, consider supporting it.
The Jersey Vindicator is an independent, nonprofit newsroom focused on accountability and transparency. Our reporting is funded by readers — not corporations, political insiders, or big advertisers.
Reader support makes this work possible — and helps ensure it continues.
Krystal Knapp is the founder of The Jersey Vindicator and the hyperlocal news website Planet Princeton. Previously she was a reporter at The Trenton Times for a decade.
